Gardasil: faith and propaganda versus hard evidence
Faith and propaganda versus hard evidence
The road to hell is paved with good intentions
In a recent news: « Cervical cancer: deaths increase as HPV vaccine is underused, says WHO »[1] published in British Medical Journal, Owen Dyer pleas for of anti HPV vaccines on the faith that this vaccine can prevent invasive cervix cancer. This golden tale is respectable but relies only on « predictions, » not on scientific hard evidences of real oncologic results. He acts as a new advocate of vaccination promising for now more than 15 years that cervix cancer will disappear in 20 years but forget to watch to oncologic results already published in cancer registries!
These real oncologic results are paradoxical and really worrying: In all the countries with high anti HPV coverage the incidence[2] of invasive cervix cancer increases in vaccinated age groups while in older (unvaccinated) population and in France, (with low vaccine coverage) the incidence diminishes.
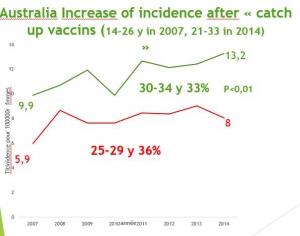
The Myth of Australian success
Australia was the first country to organize routine immunization for girls aged 12 to 26 in 2007 and is always cited as the example of success of vaccine on the belief of a simulation presented as real results[3]. But, according to the cancer register[4], vaccinated age groups women suffer from risk increase: 113% (from 0.7 to 1.5) for those aged 20 to 24 (catch up vaccinated for more than 80% of them), about a third increase for 25-29 y women (p<0.05) and for 30-34 who are less vaccinated, (p=0.01). These last increases are statistically significant and cannot be due to hazard. During the same period, most older women (and therefore unvaccinated) saw their cancer risk decrease : less 17% for women aged 55 to 59 (from 9.7 to 8.1), less 13% for women aged 60 to 64 ( from 10.3 to 8.9), less 23% for those aged 75 to 79 (from 11.5 to 8.8) and even less 31% for those aged 80 to 84 (from 14.5 to 10).
GREAT BRITAIN: THE PARADOXAL EFFECT OF GARDASIL PROMOTING CANCER
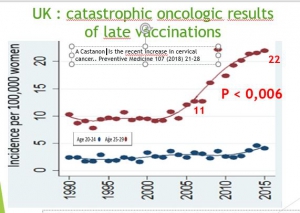
The UK national program was introduced in 2008 to offer HPV vaccination to 12–13-year-old with catch-up vaccination to girls up to 18 years old. Vaccination coverage in England has been with over 80% of 12–13-year olds receiving the full course. Coverage within the catch-up cohorts ranges from 39% to 76%). As related by Castanon « We expected cervical cancer rates decrease in women aged ages 20 to 24 from 2014… However, in 2016, national statistics showed a sharp and significant increase in the rate of cervical cancer in the vaccinated age groups. Women aged between 20 and 25 years vaccinated for more than 85% of them, saw their cancer risk increase by 70% in 2 years (from 2.7 in 2012 to 4.6 per 100,000 in 2014 p = 0.0006)[5], and those aged 25 to 30, who were aged between 18 and 23 at the time of the vaccination campaign saw their cancer risk increase by 100% between 2007 and 2015 (from 11 / 100,000 to 22 / 100,000 )”. According to Office of National Statistics Women 25 to 34 years, less vaccinated, have seen incidence increase by 18% (from 17 in 2007 to 20 in 2014). Older, women unvaccinated, benefit of stable or decreasing incidence (-13% for 65-79, 10% after 80.
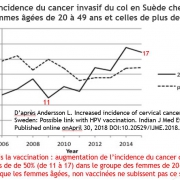
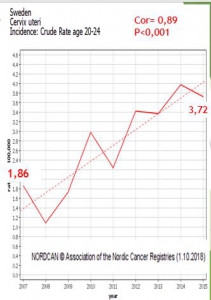
SAME PARADOXICAL PHENOMENON IN SWEDEN.
In Sweden, Gardasil has been used since 2006, and the vaccination program was rolled out in 2010, with vaccination coverage of 12-year-old girls approaching 80%. In 2012-2013, with a catch-up program, almost all girls aged 13 to 18 were vaccinated. In this country, the standardized incidence of cervical cancer in the global [6]population has increased steadily since vaccination from 9.6 per 100000 in 2006 to 9.7 in 2009, 10.3 in 2012 and 11.49 in 2015[7]. This increase is mostly due to the increase in the incidence of invasive cancers among women aged 20-24 whose incidence doubled (from 1.86 in 2007 to3.72 in 2015 c=0.89; p<0.001). The incidence of invasive cancer of the cervix increased by 24% in women aged 25 to 34 from 12.44 to 15.49(c=0.68; p=0.05), In contrast, a decrease in the incidence has been observed in women over 50. Dillner, a promoter of vaccination recognizes the increase of incidence of cancer in his country [8] but pretends that « less effectiveness of screening » is the culprit
Advocates of vaccination brandish good results against infection by stains included in the vaccines and decrease of CN2 CN3. But they should rather watch on registered cancer incidences and wonder about the paradoxical contrast of decrease of infection and statistically significant increases of invasive cancer. This paradox questions the causal Link between HPV infection and cancer and the repeated mis information pretending that 99% of cervix cancer are only due to HG HPV[9]
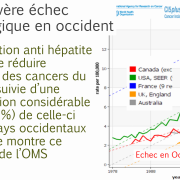
France: the bad example for big pharma
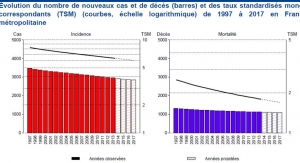
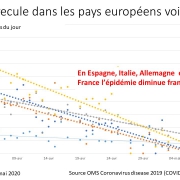
The evolution of these countries, with high immunization coverage, can be compared to the trend observed in metropolitan France, where HPV vaccination coverage is very low (around 15%). France can be considered, for this reason, as a control country. In France the incidence of cervical cancer has steadily decreased from 15 in 1995 to 7.5 in 2007, 6.7 in 2012 and 6 in 2017, much lower than the countries with high vaccine coverage. This decrease in incidence was accompanied by a decrease in mortality from 5 in 1980 to 1.8 in 2012 and 1.7 in 2017.
It is paradoxical and very worrying that this favourable French evolution, could be jeopardized by an obligation considered in the short term by our representatives[10], for some misinformed and other with too much competing interests with big pharma
[1] BMJ 2019;364: l580 doi: 10.1136/bmj. l580 (Published 6 February 2019)
[2] Incidence = number of new annual cases/100 000 women
[3] BBC Cervical cancer: Australia ‘to be first to eliminate disease’2018 10 3 https://www.bbc.com/news/world-australia-45727977
[4] Australian Institute of Health and Welfare
[5] Castanon A. Sasieni P. Is the recent increase in cervical cancer in women aged 20–24 years in England a cause for concern? Preventive Medicine 107 (2018) 21–28
[6] Cytological begnin abnormalities linked to infections
[7] According to Nordcan. register
[8] Dillner Joaquim: Livmoderhals cancer ökar hosbkvinnor med normalt cellprov Läkartidningen
Volym 115 article in swedish
[9] Ibid Already cited BBC 2018 10
[10] Their representativity is questioned by the « yellow coats